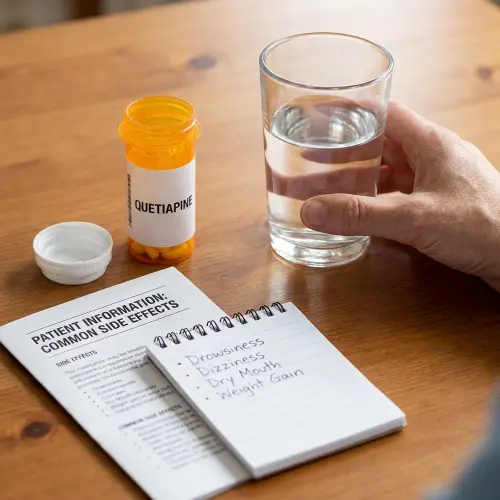
Antipsychotics night sweats can disrupt sleep. Learn causes, red flags, and cooling strategies to manage symptoms safely.
Night sweats can turn a helpful antipsychotic into a reason to dread bedtime. While the sweating itself may not be dangerous, it can wreck sleep, cause sleep disturbances, leave you dehydrated and chilled, and tempt you to skip doses of your antipsychotic medications that are keeping symptoms stable. The big problem is telling a medication side effect apart from something else, like menopause, infection, low blood sugar, or sleep apnea. Once you sort that out, you can usually make nights much more manageable without making risky changes on your own.
Yes, antipsychotics like quetiapine and olanzapine can cause night sweats by changing dopamine, serotonin, and acetylcholine signaling in the hypothalamus, the body’s temperature center. This is a well-known medication side effect that can sometimes overlap with other issues associated with various medications, including certain antidepressants, prednisone, and corticosteroids.
That’s the short version, and here’s the longer version: Many antipsychotic medications change several systems at once, and temperature regulation sits right in the middle of that overlap. Dopamine affects heat control, serotonin can influence sweating, and excessive sweating is a common complaint with several medications. Muscarinic and alpha-adrenergic effects can change how your sweat glands respond. If your body thinks it needs to dump heat, you wake up damp or drenched.
Sedation can make the situation worse, because if a medication helps you sleep more deeply, you may move less, stay buried under the covers longer, and trap more body heat in the bedding. That does not mean the drug is “too strong,” and a common misconception is that sweating is not the same thing as overdose or toxicity.
Weight gain, which can happen with some antipsychotic medications, may also increase heat retention over time. If snoring and daytime sleepiness show up too, sleep apnea can join the picture and make the sweating worse. And do not forget, other medications such as some SSRIs, commonly used antidepressants, as well as benzodiazepines, can contribute to medication side effects that include excessive sweating and sleep disturbances.
Clozapine and olanzapine are well-known examples, but risperidone, quetiapine, aripiprazole, and haloperidol can also trigger sweating in some people. There isn’t a perfect ranking, and side effects vary person to person. Clozapine has a particularly strong reputation for causing excessive sweating in some patients. Olanzapine and quetiapine are also common names in side effect discussions, partly because they affect several receptors tied to temperature and sedation. Risperidone and paliperidone can do it too, and aripiprazole may cause sweating directly, or indirectly if it causes restlessness or akathisia.
One catch is that the antipsychotic may not be the only player. If you also take sertraline, venlafaxine, mirtazapine, or other medications such as prednisone or even certain corticosteroids, the overlap can make excessive sweating more likely. Similarly, if you are on antidepressants or benzodiazepines for anxiety, the combination of medication side effects can lead to sleep disturbances and night sweats. If night sweats started after a med combination changed, not just one drug, your prescriber will want the full timeline.
Pro tip, do not assume that “newer” automatically means “less sweaty.” Side effect profiles differ, but no antipsychotic medication is completely off the hook.
Yes, you can alleviate these symptoms with some smart home cooling techniques, tighter bedding choices, and targeted airflow. One great solution is the bFan Bed Fan, which pushes room air under your top sheet to carry away body heat that gets trapped in bedding. This setup can reduce sweat-related sleep disruption without changing quetiapine or risperidone. These strategies may help counteract medication side effects that come with many medications, ranging from antipsychotics to certain antidepressants.
The goal is simple, get trapped heat away from your body before it turns your bed into a warm pocket.
Usually, yes, they are the culprit. If sweating began within days or weeks of starting risperidone or increasing olanzapine, the medication is a plausible cause, but timing matters. This assessment is similar to evaluating other medication side effects seen with a range of medications, including some antidepressants, benzodiazepines, or even prednisone.
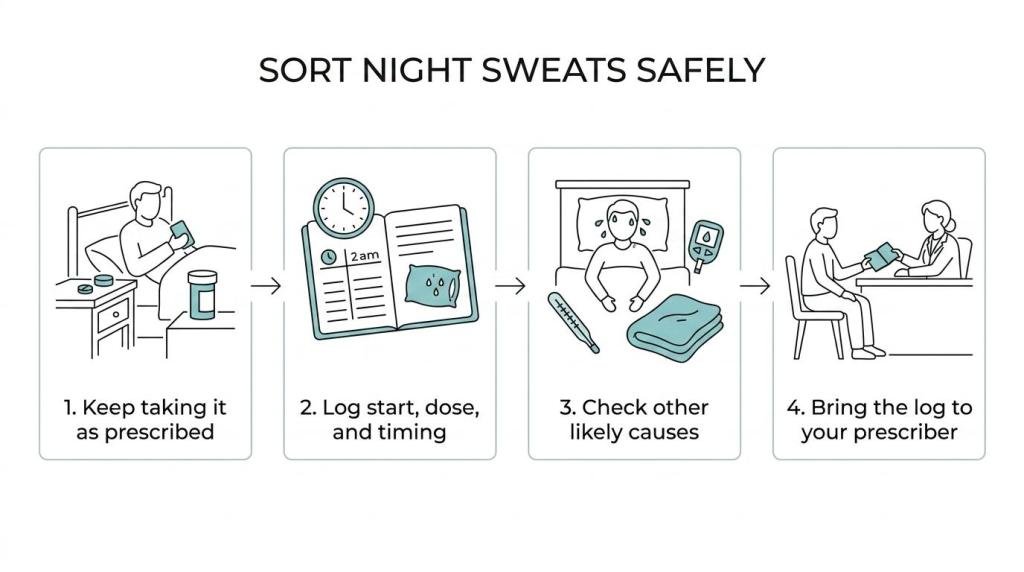
Step 1: Track the pattern, and write down when the sweating started, how often it happens, and whether it matches a dose change. For instance, if you take your medication at 9 p.m. and wake sweaty around midnight or 2 a.m. most nights, that timing is useful to note. One random sweaty night after spicy food or alcohol does not tell you much.
Step 2: Check the other usual suspects, such as menopause, infection, alcohol, anxiety, heavy blankets, low blood sugar, and sleep apnea. If you use insulin or sulfonylureas, early-morning sweats with shakiness or hunger may point toward glucose issues instead. Also, note that medications like SSRIs, benzodiazepines, prednisone, and corticosteroids may independently cause medication side effects that include excessive sweating and sleep disturbances.
Step 3: Bring the log to your prescriber, and share details like the date, dose, and pattern. If the sweating started after quetiapine went from 100 mg to 200 mg, or after clozapine was added, that’s a much stronger clue than simply saying, “I’ve been sweaty lately.”
No, do not stop quetiapine or clozapine suddenly just because sweating started after a dose change, as abrupt withdrawal can destabilize sleep, mood, or psychosis. The overlap of medication side effects—whether from antipsychotics, antidepressants, or other medications like prednisone—needs careful management.
Step 1: Keep taking the medication unless your clinician tells you otherwise, because antipsychotics and other medications are prescribed to protect against relapse, and stopping them on your own can create a much bigger problem than sweating.
Step 2: Contact your prescriber soon, and do so within the same week for bothersome night sweats. Make sure to tell them when the medication started, the current dose, whether the sweats are drenching, and whether you also have fever, rigidity, restlessness, or weight loss.
Step 3: Ask about safe adjustments, because if the medication is working well, your prescriber may weigh symptom control against comfort. That could mean watching it for another week, slowing a titration, changing the timing, adjusting the dose, or considering a switch. If psychosis or mania has just stabilized, that trade-off matters a lot.
A common misconception is that you can just cut the dose in half tonight, but that can backfire quickly.
Yes, they are different. Menopause, infection, and hypoglycemia can look similar, but patterns around quetiapine doses, fever, or insulin use often separate them. Medication-related night sweats are often tied to the timing of antipsychotic medications or other medications such as SSRIs, prednisone, or corticosteroids, and they may be regular, boringly predictable, and not tied to feeling sick during the day.
Menopause tends to bring a sudden wave of internal heat, flushing, and daytime hot flashes, too. If you are in perimenopause and taking an antipsychotic, both can be true at once.
Infections usually bring extra clues, such as fever, chills, cough, swollen glands, or generally feeling unwell. Low blood sugar often comes with shakiness, vivid dreams, hunger, palpitations, or morning confusion, especially if you take insulin, glipizide, or similar medications.
Here is a useful rule: If sweats began right after a dose change, think medication side effects; if sweats are new after months on a steady dose, think broader and get checked out.
Usually, a targeted bed cooling setup beats cooling the whole room. Both the bFan and BedJet move room air, not cold air, into the bed, which can be especially useful when managing sleep disturbances that result from various medications, including antipsychotic medications and certain antidepressants.
Sleep experts generally recommend a bedroom temperature around 60°F to 67°F. That range helps many people sleep better, but cooling the entire house all night can get expensive, especially if only one person in the bed sleeps hot. Targeted bed airflow is often more efficient because it cools the sleep microclimate instead of every square foot of the room.
Another practical point is that the original bedfan reached the market several years before BedJet was even thought of, so this style of cooling has a proven track record. If you share a bed and need separate climates, two bFans can create dual-zone control at a much lower price point. Pro tip, use a tighter-weave sheet with any under-sheet airflow system because that helps the air move across your body instead of escaping too quickly.
Yes, both your bedroom temperature and your bedding choices matter when olanzapine or clozapine leave you waking up drenched. When managing medications, including antidepressants, SSRIs, or even corticosteroids and prednisone that may cause sleep disturbances and excessive sweating, optimizing your sleep environment is key.
Step 1: Set the room within the usual sleep range. Start around 60°F to 67°F. If the room is already in that range and you are still overheating, focus next on the bed, not just the thermostat.
Step 2: Fix the bedding stack by using lighter blankets, breathable layers, and a tight-weave top sheet. If you sleep under a waterproof mattress protector, check whether it traps heat, because some do.
Step 3: Move air where the heat is trapped. A bed fan at the foot of the bed can push air between the sheets and strip away the heat pocket that builds around your torso and legs. Ceiling fans help the room, and bed airflow helps the bed.
A common miss is thinking thicker, “cooling” comforters will solve it, because if the heat is trapped under them, they may still feel hot.
Sometimes they are. Fever, rigidity, confusion, chest pain, or weight loss alongside sweating on medications like haloperidol or risperidone need prompt medical review.
Most medication-related night sweats are annoying, not dangerous. Still, some patterns deserve urgent attention because they can point to infection, neuroleptic malignant syndrome, low blood sugar, or another medical problem that should not wait.
Additionally, if you are taking other medications like benzodiazepines, SSRIs, prednisone, or corticosteroids, and you experience excessive sweating along with red flag symptoms, it is important to get prompt medical evaluation. If the sweat is truly drenching and new after months on a stable dose, that is another reason to check in with your clinician.
Yes, prescribers can sometimes reduce sweating by changing the dose, timing, or medication, but the trade-off is symptom control, especially with clozapine or olanzapine. They may also consider the overall burden of medication side effects when other medications like certain antidepressants, SSRIs, or even benzodiazepines contribute to sleep disturbances.
If sweating peaks a few hours after your bedtime dose, taking the medication earlier may help, assuming sedation will not interfere with work or evening functioning. A slower titration can also help because some side effects fade as your body adjusts.
Dose reduction is not always the answer. If a lower dose cuts the sweating but brings back hallucinations, agitation, or mania, that is not a good trade-off. Switching medications may help, though a new drug can bring its own problems, like insomnia, akathisia, constipation, or weight changes.
In some cases, prescribers consider add-on treatments for sweating. Options such as anticholinergic agents or blood pressure medications are sometimes used off-label, but they come with real downsides, including dry mouth, constipation, urinary retention, dizziness, and confusion, especially in older adults. Pro tip, ask which problem your clinician is prioritizing, be it sweat control, quality sleep, psychosis stability, or daytime function, because that makes the decision clearer.
Often, mild medication side effects such as night sweats settle within a few weeks, but persistent drenching sweats on quetiapine or aripiprazole deserve follow-up. A lot depends on what triggered the sweating. If it started with a new prescription or a dose increase, your body sometimes adapts over one to four weeks. If the sweating is still just as bad after that or worse, it is worth revisiting with your prescriber.
If you have been on the same dose for months and night sweats suddenly appear, do not assume the medication is the only reason. New alcohol use, menopause, thyroid problems, infections, diabetes changes, or sleep apnea can show up later and look like a med side effect.
If the sweating is bothersome but not dangerous, comfort measures can carry a lot of the load while you and your clinician decide what to change. If it is paired with red flag symptoms, do not wait, get checked out promptly.
Night sweats can be a nuisance when you are on an antipsychotic, but you can tackle them with some smart strategies. Consider a bedfan from www.bedfan.com as one solution, because targeted airflow from a bed fan can help you sleep cool without cooling the entire room. With timer controls to reach recommended sleep and only 18 watts on average, it’s an excellent tool to set up dual-zone microclimate control if you share a bed. Sleep experts recommend 60°F to 67°F, and with a bedfan people can often raise the room temperature by about 5°F and still sleep cool.