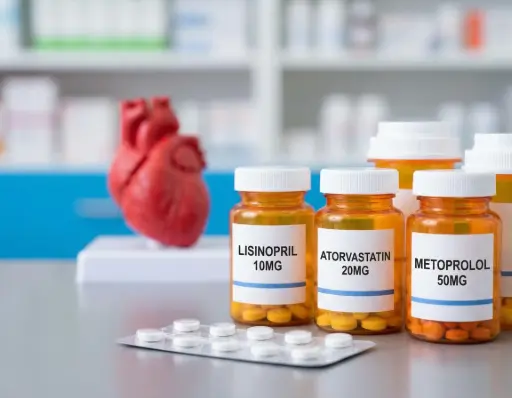
Amlodipine (Norvasc) night sweats may stem from medication, heat, or another condition. Learn causes, red flags, and cooling tips.
Night sweats can wreck sleep, raise stress, and make it hard to tell whether your blood pressure medicine is helping your health while hurting your nights. They can also compound other health concerns that many patients worry about, as detailed in your medication guide and patient information handouts. When you’re taking an oral tablet like amlodipine, commonly known as Norvasc for its role in treating high blood pressure, hypertension, and even angina, it’s important to weigh its benefits against its less-discussed common effects and side effects.
Yes, amlodipine, sold as Norvasc, can contribute to night sweats in some people, even though sweating is not one of the drug’s best-known side effects. Many patients notice that after a change in dosage or when switching from a lower to a higher dosage (for example, from 5 mg to 10 mg), they experience additional common effects such as flushing, dizziness, lightheadedness, and even nausea. If sweating starts after you begin Norvasc or following a modification in your prescribed dosage, the medication deserves a closer look alongside your other medications.
Amlodipine is a calcium channel blocker whose main job is to relax blood vessels so your blood pressure comes down and your heart has less work to do, a key benefit especially for those with coronary artery disease, heart disease, or a history of heart attack. Its standard side effects, mentioned in most patient information sheets and medication guides, include ankle swelling, flushing, headache, and dizziness. Sweating is less talked about, but it can happen, especially when vasodilation and heat sensitivity come into play.
A common misconception is that a side effect has to be common to be real, and it doesn’t. In day-to-day practice, doctors look at timing, dose changes, and the whole symptom pattern, not just whether a symptom sits in bold print on a medication guide. If you had night sweats before taking Norvasc, then the drug may not be the main cause. However, if the sweating began within days to weeks of starting it, or worsened after an increase in dosage, the connection is more likely.
It can, because amlodipine and similar medications like nifedipine widen blood vessels, which may cause flushing, warmth, and a sweat response in some people. If your body senses extra heat at night, your sweat glands may react, even if the bedroom itself is not especially warm. This effect is also observed in patients using Norvasc for angina or chest pain, who sometimes report that the medication’s side effects include heat sensations accompanied by dizziness and lightheadedness.
Think of it as a chain reaction, where blood vessels open up, skin blood flow increases, you feel warmer, and then your body tries to dump excess heat. In a cool room with loose bedding, you might barely notice it, whereas in a warmer room, or under a heat-trapping comforter, that same effect can feel much stronger. Other contributing factors may be fatigue, alcohol consumption, spicy meals, anxiety, menopause, sleep apnea, infections, and fluctuations in blood sugar, all of which can make the common effects of Norvasc and other high blood pressure medications more pronounced, especially in patients concerned about chronic health issues.
Pro tip, don’t ignore bedtime habits, because a glass of wine, a hot shower, and heavy pajamas can intensify the heat effect that sometimes accompanies a higher dosage of your oral tablet, Norvasc.
The fastest help usually comes from cooling the bed microclimate, not the whole house. Sleep experts recommend a bedroom temperature of 60°F to 67°F, and targeted airflow often lets you stay comfortable even when the room itself might be warmer. This is especially useful if you are taking Norvasc as part of your treatment for hypertension or angina.
If your prescriber wants you to stay on amlodipine despite these side effects, practical cooling tools can buy you relief right away. One solution we highly recommend is the bFan from http://www.bedfan.com.
Other cooling tips include:
You can usually narrow it down by considering the timing, pattern, and using a process of elimination. Amlodipine, menopause, and infection each tend to leave a different trail. By tracking details for a week or two, the story often becomes clearer.
%20and%20Night%20Sweats.jpg)
Side-by-side comparison of amlodipine-related night sweats, menopause, infection, and sleep apnea with their typical clues.
Start with the timeline, ask yourself when the sweats began, when you started Norvasc or had a dosage increase, and what other medications you might be using. If symptoms began soon after a new prescription or a dosage change, particularly if that change was made to better treat conditions such as high blood pressure, coronary artery disease, or angina, then that connection matters.
Next, look at the pattern, because medication-related sweating often shows up more consistently once the drug is in your routine, whereas menopause hot flashes may hit in bursts with sudden heat and flushing. Infections often include fever, chills, weight loss, and daytime symptoms.
Then check for other explanations. If you snore heavily, stop breathing during sleep, consume alcohol at night, or are on other medications that can trigger sweating (for example, certain diabetes drugs or steroids), these pieces belong in the puzzle. Common side effects from other medications can include dizziness and nausea, symptoms that could mimic those of amlodipine. Pro tip, take your temperature during an episode if you can, because if you feel drenched but don’t have a fever, it may indicate that the medication or even factors like breastfeeding could be influencing the sweating without a true infection.
They often feel different. Menopause typically causes sudden heat surges with brief episodes of flushing, while an infection tends to bring fever or make you feel generally ill. Sleep apnea is normally accompanied by snoring and gasping for air. Amlodipine-related sweating, particularly with Norvasc, is more likely to correlate with when the medication started or when its dosage was adjusted.
Menopause is one of the biggest sources of confusion here, because hot flashes can last a few minutes, wake you abruptly, and leave you throwing off covers. Amlodipine can mimic some of that because the vasodilation and flushing it causes overlap with those symptoms, and this overlap in side effects, including dizziness, fatigue, and even nausea, can complicate the patient information your healthcare provider receives.
Infection is a different category entirely. If you have a fever, shaking chills, weight loss, cough, swollen glands, or consistently drenching sweats along with chest pain, don’t assume the medication is solely responsible. Additionally, if you’re experiencing symptoms while breastfeeding or if other health concerns such as coronary artery disease or a prior heart attack are in the mix, it’s important to get checked.
Sleep apnea also deserves attention, because many people with obstructive sleep apnea wake up sweaty, especially if oxygen levels drop during sleep. If your partner notices snoring, gasping, or long pauses in breathing, it might be time to ask about a sleep evaluation.
A short symptom log helps a lot, because your clinician can make better decisions with specific dates, dosage details, and home blood pressure numbers rather than a broad “I’m sweating more.” Amlodipine and lisinopril, for instance, might be chosen differently when side effects alter the risk-benefit picture.
Keep it simple for 7 to 14 days, and write it down in your phone or on paper.
Remember, medication guides emphasize that doctors care about patterns along with isolated symptoms, so if your blood pressure is well-controlled on Norvasc even as you experience these side effects, your clinician might prefer to adjust the timing or dosage rather than switch treatments abruptly.
They solve different parts of the problem, because lowering the thermostat cools the whole room while a bed fan changes the microclimate between your sheets. Both the bFan and BedJet use room air, not refrigerated air, to alleviate the heat buildup caused by blood vessel dilation from Norvasc, and neither system actually cools the air itself.
That’s a key point, because neither device changes the temperature of the air. The BedJet doesn’t cool the air; it moves the cooler air already in the room into the bed area, and the same applies to a bed fan. If your room is 78°F, no airflow system will turn it into 60°F air, but what it does is help strip away the heat and humidity trapped around your body so you feel cooler much faster. Patients who experience side effects like dizziness or lightheadedness may find that using a bed fan mitigates discomfort without compromising their treatment for high blood pressure or angina.
Remember these key details about the bFan:
You can stack small wins, because cooler bedding, attention to dosage timing, and targeted airflow often reduce sweating the very first night. If you’re not ready to change medications, focus on improving the sleep environment first.
Start with the room, aiming for the expert-recommended 60°F to 67°F range if that’s feasible for your household. If that feels too cold or if lowering the thermostat is too expensive, using a bedfan can allow you to raise the overall room temperature by about 5°F and still sleep cool while managing common side effects, including dizziness and fatigue.
Then fix the bed itself by using a tighter-weave top sheet that lets air move across your skin and carry away heat. Avoid heavy fleece, thick toppers, or bulky comforters that trap heat, which may worsen the unwanted side effects of your oral tablet, Norvasc.
Lastly, pull back on evening triggers, avoid alcohol close to bedtime, go easy on spicy food, and opt for lighter sleepwear. If your sweating seems to worsen several hours after your Norvasc dose, ask your clinician whether adjusting the timing, perhaps taking the medication in the morning, makes sense for your treatment plan, but do not change the timing on your own. And remember, more blankets do not soak up the extra heat, they usually trap it.
Sometimes they require prompt attention, because night sweats accompanied by fever, chest pain, trouble breathing, or major swelling should not be ignored. Although Norvasc may be part of the story, serious symptoms mean you need a medical evaluation. Call your healthcare provider promptly if you experience:
If you’re breastfeeding while managing your blood pressure treatment, any new or worsening symptoms such as fatigue, nausea, or lightheadedness warrant a discussion with your prescriber.
This is why it’s smart to ask not just, "Is Norvasc causing this?" but rather, "Could something else dangerous be causing these issues too?"
Usually, you should not stop nor switch medications without consulting your prescriber. Amlodipine and other medications like losartan are both proven treatments for high blood pressure, angina, and even for reducing the risk of heart attack. The better choice depends on your blood pressure readings, dosage tolerance, kidney function, and the overall treatment plan. The medication guide and patient information provided by your clinician can help you understand these trade-offs.
If your night sweats are mild and your blood pressure remains controlled, your clinician may keep you on Norvasc and work with you to manage the symptom through lower dosage, timing adjustments, or closer evaluation of other triggers. However, if the sweating is disruptive, leading to significant discomfort, fatigue, or interference with sleep, a medication change might be advised. Alternatives include ARBs such as losartan, ACE inhibitors like lisinopril, or other classes of drugs for hypertension, each with its own set of common effects; for instance, ACE inhibitors can cause a cough while thiazides may affect your electrolyte balance.
Do not stop taking your oral tablet, Norvasc, on your own because a difficult night can lead to uncontrolled high blood pressure over the coming days or weeks. The smarter move is to bring your symptom log, blood pressure readings, and a short list of questions to your appointment, so your clinician can balance the benefits of treating coronary artery disease, angina, and even preventing future heart attacks against the current side effects you’re experiencing.
By staying informed about the common effects, side effects, and potential health concerns detailed in your medication guide and patient information, you can work with your healthcare provider to maintain effective treatment while minimizing the downsides.