
Pralatrexate night sweats may stem from treatment, lymphoma, or infection. Learn warning signs, when to call your oncologist, and how to sleep cooler.
Night sweats during cancer treatment can wreck sleep, sap energy, and make every treatment cycle feel harder than it already is. With pralatrexate, the real problem is not just the sweating itself, it’s figuring out whether it’s a manageable side effect or a clue that something more serious is going on. If you’re taking pralatrexate for peripheral T-cell lymphoma, you need a clear way to sort out the cause, know when to call your oncology team, and get cooler at night without guessing.
Yes. Pralatrexate, sold as Folotyn, can overlap with night sweats, but it is not usually one of the headline toxicities or side effects like mucositis or low blood counts are. In people with peripheral T-cell lymphoma, sweating may come from the drug, the cancer, or an infection.
That distinction matters. Pralatrexate is an antifolate chemotherapy used most often in relapsed or refractory peripheral T-cell lymphoma. During treatment, your body can sweat more at night for several reasons, including fever, immune signaling, anxiety, steroid premeds, birth control, or heat getting trapped under bedding when you’re already sleeping warmer than usual.
A common mistake is blaming every symptom on the infusion. If the sweats are new, drenching, or paired with chills, you should think beyond the drug itself.
They usually happen through temperature dysregulation, not because pralatrexate directly “creates heat.” Cytokines, dexamethasone, and active lymphoma can all shift how your hypothalamus handles body temperature. If your body is fighting inflammation or infection, sweating is one way it dumps heat.
Here’s the practical version. If pralatrexate irritates tissues, lowers blood counts, or leaves you more vulnerable to infection, your system can respond with feverish swings or heat surges at night. If lymphoma is still active, inflammatory signals can keep your internal thermostat running high even when the room feels normal.
Folic acid and vitamin B12 are standard with pralatrexate because they help reduce some toxicities, especially mouth sores and blood count problems. They are not a treatment for night sweats. If sweating improves after bedding changes but not after treatment adjustments, trapped heat may be a bigger driver than the drug.
The best options remove heat close to your skin, not just from the room. bFan, tight-weave sheets, and moisture-wicking sleepwear usually work better together than any single fix alone. If your sweating is treatment related, a layered setup often gives the fastest relief.
You want less trapped heat, less soaked fabric, and less disruption at 2 a.m. That usually means targeting the bed microclimate instead of overcooling the whole house.
Sleep experts usually recommend a room temperature between 60°F and 67°F. With a bed fan, many people can raise the room temperature by about 5°F and still sleep cool, which can lower air conditioning use.
You can often tell by the pattern. Pralatrexate related sweating tends to cluster around treatment days, lymphoma sweating is often persistent and drenching, and infection usually brings fever or chills. Pralatrexate and neutropenia raise the stakes because infection can turn urgent fast.
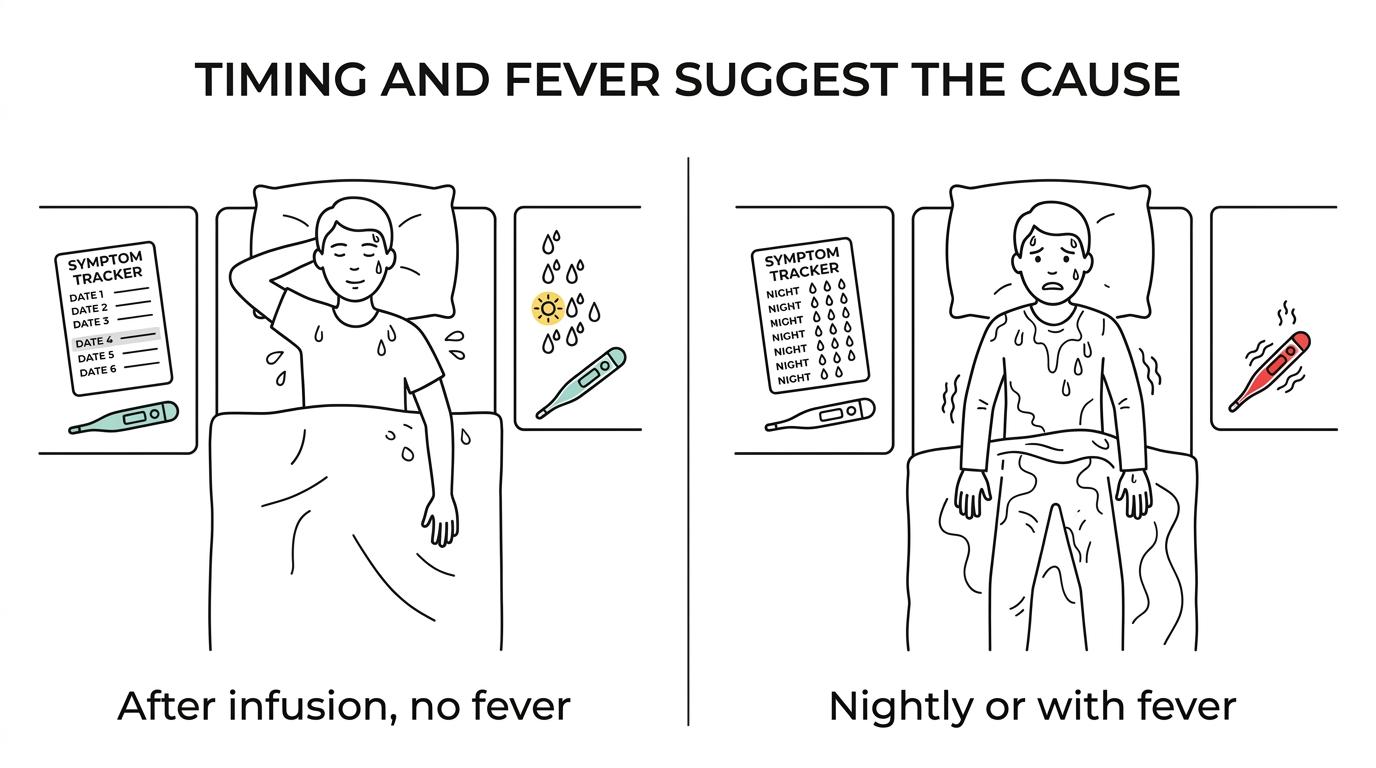
If the sweats started soon after beginning treatment, appear in the first few days after each infusion, and come without fever, they may be treatment associated. If they’re happening every night, soaking the sheets, and you’re also losing weight or noticing enlarged nodes, active lymphoma moves higher on the list.
Infection is the one you do not want to miss. If sweating comes with a temperature of 100.4°F or higher, shaking chills, cough, burning urination, or feeling suddenly unwell, call your oncology team the same day. A common misconception is that infection always looks dramatic. During chemotherapy, it can start subtly.
Start with safety first. Check your temperature, change into dry layers, and take stock of any chills, cough, or mouth sores. Pralatrexate and a digital thermometer are a better first move than guessing whether you should “wait and see,” especially when considering potential side effects.
First, take your temperature before you do anything that could hide a fever. If it is 100.4°F or higher, or you have shaking chills, call your oncology team right away.
Second, swap out wet clothing and pillowcases, especially if you've recently started or stopped using birth control, as hormonal changes may affect sweating. A dry surface stops evaporative chill, which is the miserable cold feeling that often follows heavy sweating.
Third, drink some water if you can keep fluids down. If you’re dealing with mouth sores from pralatrexate, which can be potential side effects, take small sips or use ice chips if your care team allows them.
Fourth, note the time, how severe it was, and whether you’re near an infusion day. If it happens again, that pattern helps your oncologist decide whether to check labs, cultures, or imaging.
A useful tip here, don’t pile on heavy blankets after a sweat episode just because you feel cold for a few minutes. That often traps the same heat again and starts the cycle over.
They are urgent when they pair with fever, chills, or signs of infection. Pralatrexate, low neutrophils, and oral mucositis can make a small infection become a big problem quickly due to potential side effects. Same-day reporting is standard oncology practice, not overreacting.

Night sweats alone are uncomfortable. Night sweats plus red flags can signal neutropenic fever, pneumonia, a urinary infection, dehydration, or disease activity that needs prompt review.
Watch for combinations like these:
If one of those shows up, then the goal changes. You’re no longer just managing sleep comfort, you’re screening for a complication.
A short symptom log is one of the fastest clinical tools you can create. Your oncologist, infusion nurse, and CBC results make more sense when the sweats are tied to exact days, temperatures, and other symptoms. Good tracking often shortens the time to a useful decision.
Start by logging the date, the time you woke up, and whether your shirt or sheets were damp, wet, or soaked. Keep it simple. A one-line note is enough if you do it consistently.
Then add context. Write down your last pralatrexate infusion date, any steroids or anti-nausea medicines you took, your bedtime room temperature, and whether you had alcohol, spicy food, or a very heavy blanket. Those details help separate treatment effects from ordinary heat triggers.
After that, connect the sweats to other symptoms. If they happen with mouth sores, low appetite, diarrhea, fatigue, or any side effects from medication, your team may look more closely at dehydration or overall treatment tolerance. If they happen with fever or chills, the next step may be urgent labs or cultures.
Pro tip, don’t wait for a “perfect” journal. Three or four accurate entries are more useful than trying to remember two weeks of rough nights from memory.
A bed fan is usually the more efficient targeted option for personal comfort, while whole-room cooling is broader but costlier, much like choosing birth control methods tailored to individual needs. bFan and BedJet both use the air already in your room, they do not cool the air themselves. That means performance depends on room temperature, sheet type, and airflow under the covers.
Here’s the trade-off. Lowering the thermostat cools the whole space, which can help if your bedroom is genuinely too warm. But if only you are overheating, it can waste energy and make your partner uncomfortable.
A bed fan targets the microclimate around your body, minimizing potential side effects associated with whole-room cooling. That’s often more useful during chemotherapy, when your core issue is trapped heat under bedding. The original Bedfan came to market several years before BedJet was even thought of, and the basic idea still holds up well, move room air through the bed, not through the whole house.
bFan has a few practical advantages for many shoppers:
One common misconception is that these systems are air conditioners. They aren’t. Neither bFan nor BedJet cools the air. They both use the cooler air already in the room and move it under the covers, which is why sleep experts’ 60°F to 67°F range still matters.
The best setup controls heat, moisture, side effects, and disruption all at once. A cool room, tight-weave sheets, and a consistent bedtime setup beat random gadget swapping. If your night sweats are frequent, routine matters almost as much as the cooling tool.
Start with the room. If you can, keep it in the 60°F to 67°F range sleep experts recommend. If that feels too cold for the household, a bed fan often lets you raise the room temperature by around 5°F and still sleep cooler.
Next, tune the bed. Use a breathable fitted sheet, a tight-weave top sheet, and the lightest blanket you can tolerate. If you use a bed fan, this is where sheet choice matters. Tight-weave fabric helps the air travel across your body and carry away heat.
Then set up for interruptions. Put water, a clean shirt, and a towel within reach. If you use a bFan or similar bed fan, use the timer controls so the airflow matches the part of the night when you typically overheat. That small change can reduce how often you fully wake up.
A practical misconception to drop, “more airflow is always better.” Sometimes medium airflow is more comfortable than maximum, especially if you get chilled after sweating.
The symptoms around the sweat episode often tell the real story. Fever, swollen nodes, and weight loss point one way, while mouth sores, diarrhea, and dehydration point another. Pralatrexate, lymphoma, side effects, and infection each leave different clues if you look at the full picture.
This is where pattern recognition helps you and your care team most:
If your sweats are isolated and improve with better bed cooling without any side effects, that’s reassuring, but it doesn’t replace clinical judgment. If they’re getting worse, pairing with fever, or showing up alongside new symptoms, then the safer move is to call, report the pattern clearly, and let your oncology team decide the next step.