Hydralazine night sweats may stem from vasodilation, other meds, or sleep conditions. Learn causes, cooling tips, and when to call a doctor.
Hydralazine can be very effective for high blood pressure treatment, but some people notice an annoying side effect once the lights go out, they wake up hot, damp, and wide awake. That matters because broken sleep can raise daytime fatigue, worsen mood, and make high blood pressure harder to manage the next day. The real challenge is figuring out whether the sweating is coming from hydralazine itself, another medication like hydrochlorothiazide or an added diuretic, a health issue, such as heart failure, kidney failure, liver disease, or even a sleep setup that traps heat. Once you sort out the cause, you can usually make nights much more manageable.
Yes, hydralazine can trigger night sweats, and the likely driver is vasodilation in your skin blood vessels, not heat production from the drug itself. These side effects—even including headache, nausea, and dizziness—can affect your overall treatment experience.
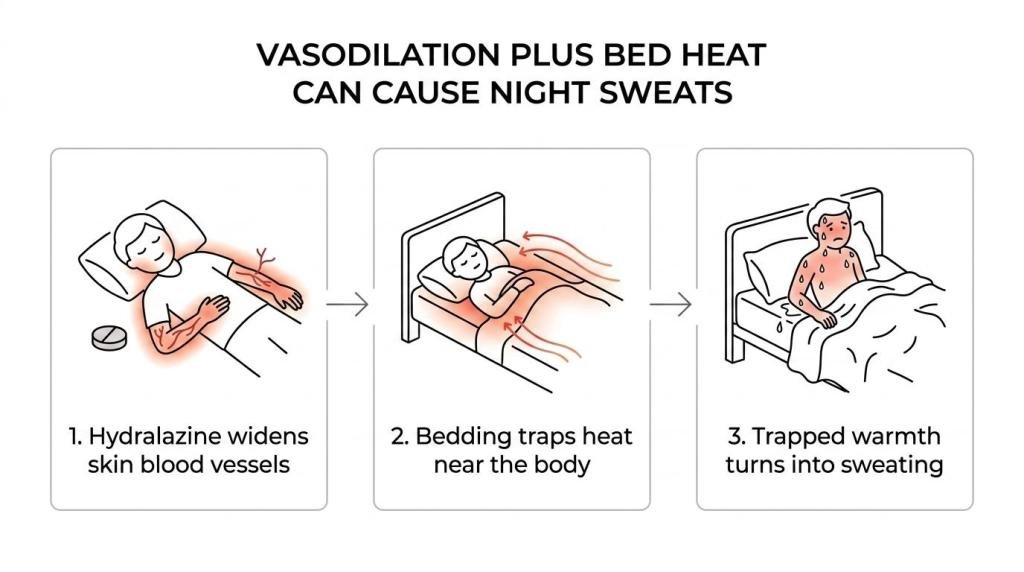
Hydralazine relaxes blood vessels so blood can flow more easily. That helps lower blood pressure but can also increase blood flow near the skin, which can make you feel flushed or warm. If your bedding already traps body heat, that warmth can turn into sweating once you’re under the covers.
Night sweats also tend to feel worse than daytime sweating because your mattress, comforter, and sleepwear hold heat close to the body. A common misconception is that sweating always means the drug is “too strong” or that you’re having an allergy. Sometimes it’s simply a heat-management problem caused by the medication plus your sleep environment, especially when additional treatments (such as hydrochlorothiazide or other diuretics) are part of your high blood pressure regimen.
Hydralazine-related sweating is real, but it is not usually listed as the drug’s most common complaint in patient guidance from sources like the FDA and Cleveland Clinic. It is one of several side effects that patients might experience, alongside potential headache, nausea, and dizziness.
That means two things. First, if you’re sweating at night on hydralazine, you’re not imagining it. Second, it’s still worth checking whether something else is contributing, because drenching sweats are not specific to one medication. This is especially important if you are being treated for conditions like heart failure, kidney failure, or have had a stroke.
The severity of side effects matters more than their frequency. Mild sweating that started after a dose increase is very different from soaking sweats with fever, weight loss, or chest pain. If your sleep is getting wrecked several nights a week, the side effect is serious enough to address, even if it is not dangerous in an emergency sense.
Absolutely, menopause, SSRIs, thyroid problems, low blood sugar, and sleep apnea are all common causes that can overlap with hydralazine. In addition, other medications, including hydrochlorothiazide (a diuretic commonly used with hydralazine to manage high blood pressure), may contribute to similar side effects, as may potential interactions between multiple medications.
This is where timing helps. If the sweating began right after starting hydralazine, or after the dose was raised, the medication moves higher on the list. If you’ve been stable on the same dose for months and suddenly develop drenching sweats, look wider.
Other medication triggers are common. Antidepressants like sertraline and fluoxetine, steroids like prednisone, and diabetes drugs that can cause nighttime hypoglycemia are frequent offenders. Hormonal shifts, especially perimenopause and menopause, are another big one. If you snore, wake unrefreshed, or gasp at night, obstructive sleep apnea can also show up with sweating.
That’s why the question is not just, “Can hydralazine do this?” It’s, “Is hydralazine the main reason this is happening right now?” Also, consider that pediatric patients and individuals who are breastfeeding may have specific considerations when it comes to both high blood pressure treatment and medication interactions.
Targeted cooling usually works better than just making the whole house colder, especially when trapped bedding heat is the main problem.
The goal is simple: move heat and moisture away from your skin fast enough that your body can settle back into sleep, minimizing any side effects from medication. That can mean changing the room, the bed, the bedding, or the medication plan. In practice, the best results usually come from combining two or three small fixes instead of chasing one perfect solution.
Timing gives the best clue, and a simple log with hydralazine doses and bedtime symptoms can separate medication sweating from menopause, SSRIs, or infection.
Start with three nights of notes to track any potential side effects, a week is even better. Write down when you took hydralazine, what time you went to bed, room temperature, alcohol intake, and whether you woke sweaty. Add blood pressure if you monitor at home.
Step 1 is pattern matching. If sweats begin 1 to 4 hours after your evening dose, the medication becomes a stronger suspect. Step 2 is context. If your room was 74°F, you drank wine, and you used a heavy duvet, the medication may only be part of the story. Step 3 is consistency. If the sweats happen on cool nights too, or after every dose increase, that’s useful evidence for your prescriber about potential side effects.
Practical tip, don’t skip or double up hydralazine on your own just to “test” the theory. That can create blood pressure swings and muddy the picture.
Cool the bed first, not just the room, and use dry fabric, water, and airflow before you jump to medication changes.
Step 1, get the moisture off your skin. Swap a damp shirt or pillowcase for a dry one, and push back the top layer of bedding for a minute or two. Even a brief reset helps your body stop chasing heat.
Step 2, create airflow where the heat is trapped. If you have a bed fan, turn it on or increase it for 10 to 20 minutes. If not, aim a room fan across the bed while you uncover briefly. This is where under-sheet airflow usually wins, because it reaches the sweaty zone instead of just moving air near your face.
Step 3, check how you feel overall. If you’re sweaty but otherwise okay, that’s one thing. If you’re dizzy, faint, short of breath, or your heart is racing, check your blood pressure if you can and seek medical advice.
A bed fan is usually more energy-efficient than dropping central AC, and sleep specialists still point to 60°F to 67°F as the best room range.
Lowering the thermostat cools the whole room, which helps, but it can cost a lot if you only need cooling in one bed. A bed fan tackles the microclimate inside the sheets, where your body heat actually gets trapped. That’s why many hot sleepers can keep the room about 5°F warmer and still stay comfortable.
There is a trade-off. A bed fan does not cool the air. It only uses the cooler air already in the room to cool your bed, the same basic limit as a BedJet. If your bedroom is hot and humid, say 78°F with poor AC, no bed airflow device can fully make up for that. You still need a reasonably cool room.
A useful misconception to clear up: more airflow is not the same as more noise. At normal operating speed, a Bedfan is typically in the 28 dB to 32 dB range, which is quiet enough for many bedrooms.
Both Bedfan and BedJet move room air into the bed, but price, simplicity, and zoning are where the choice changes.
The first thing to know is that neither product cools the air. The BedJet doesn’t cool the air, and the Bedfan doesn’t either. Both rely on the cool air already in the room and then direct it into the sleep space.
The original Bedfan came to market several years before BedJet was even thought of, and the concept is still pretty straightforward: remove trapped body heat from under the covers. Where the comparison gets practical is cost and setup. One BedJet is more than twice the price of a single Bedfan. The dual-zone BedJet is over a thousand dollars and more than twice the price of two Bedfans.
If you sleep with a partner and need two different cooling zones, the bFan can create dual-zone microclimate control using two fans, one for each sleeper. If you want a more feature-heavy system, a different product may appeal to you. If your main goal is simple, quiet, lower-cost relief for medication-related overheating and avoiding side effects, the Bedfan is often the easier answer.
Your sheet fabric and airflow path matter more than most people think, and cotton percale or another tight-weave sheet usually works best with under-sheet airflow.
Step 1, get the room into a realistic sleep range. Sleep experts recommend 60°F to 67°F. If that feels too cold for the household, start a few degrees higher and use targeted bed cooling to bridge the gap.
Step 2, choose bedding that lets air travel across your body. Tight-weave sheets work well because they guide air under the covers instead of letting it dissipate. This surprises people, but very open, fluffy, or plush layers can actually weaken the cooling effect.
Step 3, use timing to your advantage. Many people overheat most during sleep onset and the first part of the night. A bed fan with timer controls lets you start cooler, then taper later so you don’t wake up chilled at 4 a.m.
Call sooner if night sweats or side effects come with fever, rash, chest pain, or unexplained weight loss, because hydralazine can overlap with problems that need medical review. Also, if you experience persistent headache, nausea, or dizziness—especially if you are taking other treatments like hydrochlorothiazide or managing conditions such as liver disease—seek advice immediately.
Most medication-related sweating is annoying, not dangerous. But some combinations of symptoms change the picture. Hydralazine has rare but important immune-related side effects, including lupus-like reactions in some long-term users, and those can involve fever, joint pain, and feeling generally unwell.
Watch for patterns like these:
If you have diabetes, add nighttime glucose checks to the conversation, because hypoglycemia can feel a lot like a medication sweat episode.
Yes, a clinician can sometimes adjust timing, dose, or the drug plan, but the right move depends on your blood pressure, kidney function, liver disease status, and why hydralazine was prescribed. Sometimes the fix is simple. Moving the timing, splitting doses differently, or adjusting another blood pressure medicine such as hydrochlorothiazide can reduce nighttime symptoms without losing effective high blood pressure treatment. In other cases, your prescriber may decide another medication class fits better—especially if you are in a pediatric situation or are breastfeeding where specific precautions are necessary.
Bring useful data to that visit. A symptom log, home blood pressure readings, medication timing, and notes about room temperature can make the conversation much more productive. If the sweats mainly happen when your room is warm, then cooling the bed may solve most of the problem. If they happen regardless of room conditions, then a medication change becomes a stronger possibility.
Either way, it helps to solve the sleep problem from both ends, talk to the prescriber about the drug, and make the bed environment work for you instead of against you.