
Cortisone night sweats can disrupt sleep by altering heat regulation. Learn common causes, quick relief tips, and when to call a doctor.
Cortisone night sweats can turn a medication that calms inflammation into a rough cycle of overheating, wake-ups, and poor recovery. The problem is bigger than damp sheets, broken sleep can worsen pain, mood, concentration, and next-day fatigue. Many people need cortisone, prednisone, or related corticosteroids for asthma, joint pain, autoimmune flares, or skin conditions, so the real fix is not “just stop the medicine.” It’s figuring out why the sweating is happening, how to reduce it fast, and when it points to something more serious.
Yes. Cortisone and prednisone can trigger night sweats, excessive sweating, and hyperhidrosis by affecting thermoregulation, blood sugar, hormones, and sleep depth, especially when doses are taken later in the day.
Cortisone is a corticosteroid, also called a glucocorticoid, similar to prednisone. Drugs in this class can make your body feel warmer, increase alertness, and shift how blood vessels respond. If your dose peaks near bedtime, you may notice flushing, restlessness, or sweating after you first fall asleep.
There’s another layer. Steroids and certain medications can raise blood glucose in some people, and glucose swings can leave you sweaty and uncomfortable overnight. That matters even more if you already have diabetes, prediabetes, or you’re taking other meds that affect blood sugar.
A common misconception is that sweating means the drug, such as prednisone, is “heating the room.” It isn’t. The drug is changing how your body handles heat and sleep. If the timing matches your dose, especially after a new prescription, dose increase, or cortisone injection, the medication is a very plausible trigger.

Usually, they’re a known side effect, but fever and TB are red flags. Night sweats after cortisone are often benign, yet steroids can also mask infection.
If the sweats started soon after cortisone and you feel otherwise okay, they’re often more annoying than dangerous. Still, context matters. Steroids suppress immune responses, which means you can be sick without the usual obvious fever. That’s why night sweats on cortisone deserve a little more respect than random overheating on a warm night.
Watch the pattern. If the sweats happen only on treatment days, or within 24 to 72 hours after an injection, a medication effect is likely. If they’re getting heavier, happening with cough, weight loss, swollen lymph nodes, or chest symptoms, think beyond the drug.
Pro tip, keep a simple log for three nights. Record dose time, bedtime, wake-ups, room temperature, and whether the sheets were damp or soaked. That one-page note often tells your healthcare provider more than a vague “I’m sweating a lot.”
The best fixes reduce trapped heat fast. bFan Bed Fan and tight-weave cotton sheets usually work better than piling on colder room air alone.
If your main problem is heat building up under the covers, targeted airflow tends to work better than trying to turn the whole bedroom into a refrigerator. That’s where a few practical changes can make a real difference, starting tonight.
Timing usually gives it away. Cortisone, prednisone, certain medications, menopause, and SSRIs can all cause night sweats, but their patterns are often different.
Cortisone and prednisone are in the same family, so the main difference is often dose strength, duration, and when you take them, not whether one is magically sweat-free. If your symptoms, such as excessive sweating or hyperhidrosis, started after new medications, a steroid injection, an oral burst, or a dose increase, that’s a strong clue.
If the sweating was there before steroids, consider other potential treatments and look wider. Menopause, infection, anxiety, obstructive sleep apnea, acid reflux, and antidepressants like Lexapro or Zoloft can all show up as night sweats. If sweats happen only during hot flashes, shifts in hormones may be more likely. If they come with snoring, choking awake, or morning headaches, sleep apnea moves up the list.
Here’s the practical rule. If the symptom starts after the medicine starts, gets worse after a dose increase, and eases as the steroid effect fades, prednisone or cortisone is a likely driver. If it ignores that pattern, your healthcare provider should check for another cause, or more than one cause at the same time.
Start with targeted cooling. A cool room and directed airflow, from a bed fan or ceiling fan, usually work faster than changing blankets over and over.
Step 1, cool the sleep zone, not just the house. If your room is already within the sleep-friendly range of 60°F to 67°F, focus on moving that air under the covers. That’s why bed cooling systems help so much with prednisone-induced steroid sweats, the heat is usually trapped between your body and bedding.
Step 2, reduce heat trapping. Use lighter sleepwear, one breathable top sheet, and avoid stacked blankets. If you use a bed fan, tighter-weave sheets usually spread the air better across your body. Many people assume looser bedding always feels cooler, but airflow control matters more than fluffiness.
Step 3, prevent the rebound chill. Put a dry shirt by the bed, wipe down quickly, drink a few sips of water, and get back under a dry layer. That keeps one hot episode from turning into an hour of feeling clammy and awake.
Be specific. Prednisone, hydrocortisone, and cortisone side effects are easier to fix when your clinician can see the timing, dose, and severity clearly.
Step 1, bring the pattern. Note the exact drug, dose, how you take it, what time you take it, and when the sweating starts. Include whether you had a cortisone injection, oral tablets, or both. Also note fever, cough, glucose issues, or insomnia.
Step 2, ask targeted questions. Could morning dosing help, if your condition allows it? Is the dose higher than needed? Would a shorter taper, a different steroid, or a nonsteroid option be reasonable? If you have diabetes risk, ask whether glucose checks make sense.
Step 3, don’t stop abruptly unless you’re told to. That’s the big misconception. People get miserable and want off the drug immediately, but sudden steroid withdrawal can be risky, especially after longer courses. The trade-off is simple, symptom relief matters, but safe tapering matters more.
Usually, yes, if trapped bedding heat is the main issue. bFan and BedJet both move room air, but neither one cools the air itself.
Lowering the thermostat can help, especially if the whole room is hot and humid. The downside is cost, partner comfort, and overcooling the room when the real problem is heat trapped under the covers. That’s common with prednisone-related sweating, because you may feel fine in the room and still overheat inside the bed.
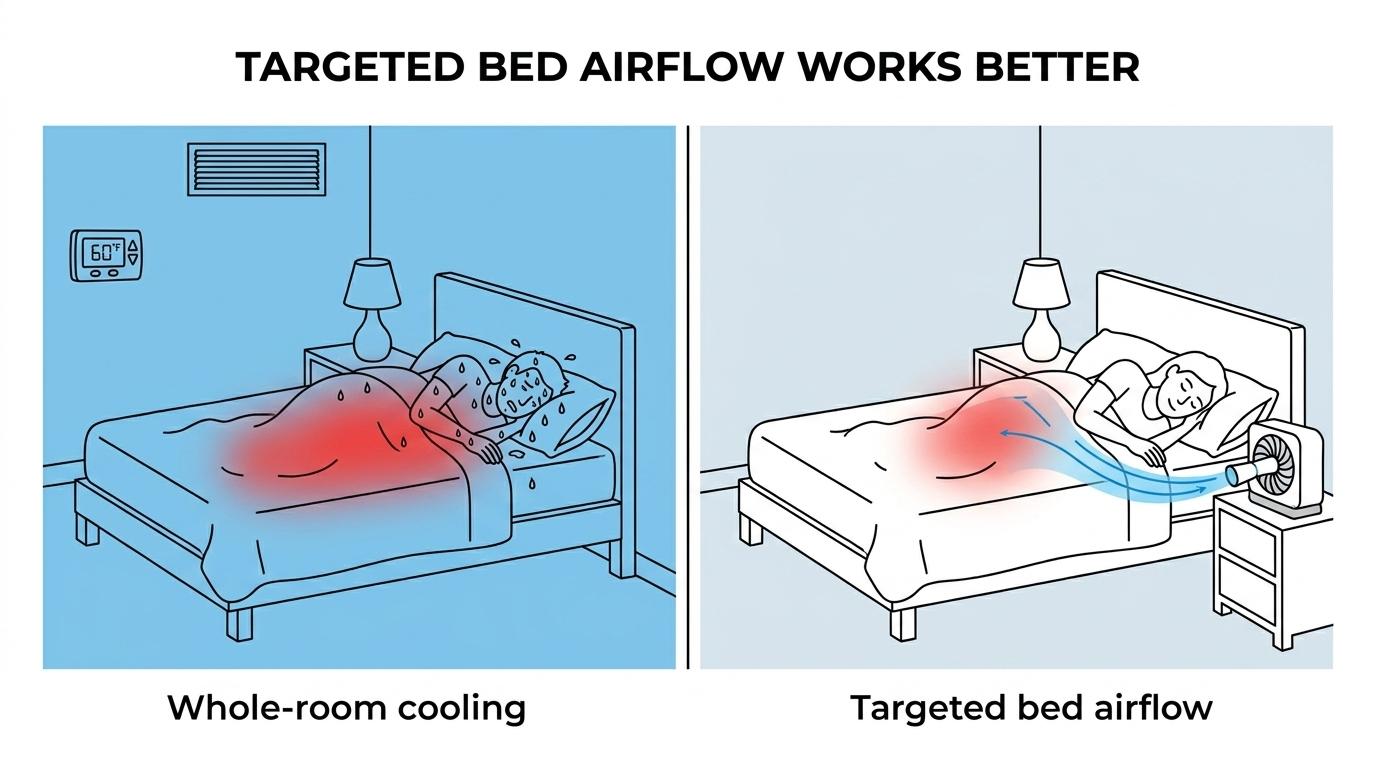
A bed fan targets the microclimate around your body. That usually means faster relief, less AC use, and fewer middle-of-the-night blanket battles. With bFan, people can often raise room temperature by about 5°F and still sleep cool, which can cut cooling costs without losing comfort.
After you think about the trade-offs, the choice usually looks like this:
They matter a lot. Cotton percale and a breathable mattress surface often outperform heavy bamboo blends or plush toppers when sweating is your main problem.
Your bedding can either release heat or trap it. Tight-weave sheets are usually best with a bed fan because they help the air travel across your body and carry away heat. That sounds backwards to some people, but a controlled air channel often works better than a loose weave that lets the airflow dissipate.
Pajamas matter too. Light, moisture-wicking fabrics help if you sweat heavily or have hyperhidrosis, but thick “cozy” sets often make prednisone-induced steroid sweats worse. Waterproof mattress protectors, memory foam toppers, and heavy duvets can also hold heat against you.
A smart setup is simple, breathable sheets, one light layer, steady air movement, and reasonable humidity. If your room feels sticky, even a good cooling strategy will struggle. Aim for a dry, cool room first, then fix the bed microclimate.
Seek care quickly if night sweats come with fever, chest pain, or confusion. Cortisone can hide infection signs, so don’t wait on serious symptoms.
This is where people sometimes get too casual. Prednisone side effects are common, but night sweats can also show up with pneumonia, tuberculosis, bloodstream infection, blood sugar problems, and a few cancers. The point isn’t to panic, it’s to notice when the picture doesn’t fit a simple medication side effect or when medications might be interacting in unexpected ways.
Call a clinician promptly, or seek urgent care, if you have any of these:
A repeatable plan works best. Cortisone, menopause, and sleep apnea often overlap, so one fix usually isn’t enough by itself.
Step 1, map your pattern across treatment cycles. Do the sweats happen after injections, oral tapers, late doses, or only during disease flares? If the pattern repeats, you can prepare before the bad nights start.
Step 2, lock in a standard sleep setup. Keep the room in the 60°F to 67°F range when possible, use breathable bedding, and add targeted airflow under the covers. If steroid sweats are predictable, set timer controls on your bed fan so cooling matches the hours when you usually overheat and still supports the recommended sleep window.
Step 3, check for stacked causes. If you also snore, have reflux, take medications like antidepressants, or you’re in perimenopause, steroids may be only one piece of the problem. When the pieces connect, treatments get more accurate, and sleep usually improves faster.
Cortisone night sweats are episodes of excessive sweating during sleep that can occur when someone is taking cortisone or other corticosteroid medications. These medications can disrupt your body’s natural hormone balance, which may lead to increased sweating at night. Many people find these night sweats uncomfortable and disruptive to their sleep, making it important to find effective ways to manage them.
Cortisone can affect your body’s hypothalamus, which is the part of your brain that controls temperature regulation. When you take cortisone, it can throw off your body’s normal temperature control, leading to increased sweating, especially at night. This side effect is fairly common and can be more noticeable if you are taking higher doses or have just started the medication.
The duration of cortisone night sweats varies from person to person. Some people experience them only during the initial days or weeks of starting cortisone therapy, while others may have them for as long as they are on the medication. Once the dosage is reduced or the medication is stopped, night sweats usually improve, but it can take a few days to a few weeks for your body to adjust.
Cortisone night sweats are generally not dangerous, but they can be very uncomfortable and may disrupt your sleep. If you experience other symptoms like fever, chills, or unexplained weight loss along with night sweats, it’s important to contact your healthcare provider. These symptoms could indicate an underlying infection or another medical issue that needs attention.
There are several ways to manage cortisone night sweats at home. Keep your bedroom cool, use breathable bedding, and wear lightweight pajamas. Sleep experts recommend keeping your room between 60°F and 67°F for optimal sleep, and with a bedfan, you can often raise your room temperature by about 5°F and still sleep cool. The bFan from www.bedfan.com is a great solution, offering dual-zone microclimate control and timer controls to help you stay comfortable all night.
Yes, changing your bedding can make a big difference. Choose sheets with a tight weave, as they help air flow across your body and carry away heat more effectively. Lightweight, moisture-wicking fabrics are also helpful. Pairing these sheets with a bedfan can further improve airflow and comfort, making it easier to manage night sweats.
While both cortisone and menopause can cause night sweats, the underlying causes are different. Cortisone night sweats are triggered by medication affecting hormone balance, while menopause night sweats are due to natural hormonal changes in the body. The symptoms can feel similar, but the management strategies are often the same, focusing on cooling the sleeping environment and improving airflow.
Absolutely, there are several products designed to help with night sweats. The bFan, also known as a bedfan, is highly recommended because it uses only 18 watts on average and operates quietly at 28db to 32db. It was on the market years before other options like Bedjet, and it’s more affordable, with a dual-zone Bedjet costing over a thousand dollars, which is more than twice the price of two bedfans. The bFan doesn’t cool the air but uses the cool air in your room to keep you comfortable, making it a practical and energy-efficient solution.
Yes, you should always let your doctor know if you’re experiencing side effects like night sweats from cortisone. Your doctor may be able to adjust your dosage or suggest other ways to manage the symptoms. Never stop or change your medication without consulting your healthcare provider, as they can help you find the safest and most effective approach.
All links have been checked and are currently working, leading to authoritative and up-to-date resources.