Valsartan night sweats may happen, especially with dose changes or dehydration. Learn causes, warning signs, and practical relief tips.
Night sweats can wreck sleep, spike anxiety, and make it hard to tell whether your blood pressure medicine is bothering you or something else is going on. With valsartan, the main problem is uncertainty, because sweating at night is possible, but it is not one of the best-known side effects people expect. Be aware that valsartan is associated with a spectrum of side effects, ranging from minor discomfort to more noticeable symptoms. If you’re waking up hot, damp, or soaked, you need a practical way to sort out likely medication effects from red flags, while still getting some sleep tonight.
Yes, valsartan and Diovan can be linked to night sweats, although the FDA labeling does not list them as a top common side effect. While night sweats are not among the most commonly reported side effects, some patients may also experience dizziness as a side effect. That matters because "not common" does not mean "never happens." Real-world medication effects often show up as patterns, not neat checkboxes. If your sweating started soon after you began valsartan, or after your dose went up, the medication moves higher on the suspect list.
A common misconception is that only drugs famous for sweating, like SSRIs or steroids, can trigger nighttime overheating. In practice, blood pressure medicines can still be part of the picture, especially when they change circulation, hydration, or how warm you feel at night.
Valsartan is an ARB, short for angiotensin II receptor blocker, and it is commonly prescribed to manage hypertension. It is widely used for high blood pressure, heart failure, and heart protection after certain cardiac events. Most people tolerate it well, but side effects do vary from person to person.
Valsartan can change blood vessel tone and fluid balance, and your body may answer with sweating, especially when hydrochlorothiazide or alcohol is also involved. Valsartan relaxes blood vessels by blocking angiotensin II at the receptor level, which lowers blood pressure, but it can also shift how your body handles heat, circulation, and nighttime comfort. If you already sleep warm, a small change can feel much bigger once you’re under blankets.
Here’s the connection in plain language. If valsartan lowers your pressure a bit more at night, then your body may respond by nudging your autonomic nervous system. That can mean a flushed feeling, mild clamminess, or full-on sweating in sensitive people. Other possible side effects may include mild nausea and vomiting, although these are less frequently reported. It is also important to note that individuals with a history of allergies should inform their doctor, since side effects may become more pronounced in those cases. Dehydration can make it worse. If you take valsartan with a diuretic, or you drink alcohol at dinner, or your room is too warm, then the sweating may become more obvious. That does not prove valsartan is the only cause, but it does explain why the symptom often shows up as a stack of small factors rather than one dramatic trigger.
Keep in mind that sweating alone does not automatically mean an allergy. Allergic reactions usually bring other signs, like rash, swelling, wheezing, or facial puffiness.
The best first moves are safer sleep cooling, hydration checks, and medication review, with the bFan from Bedfan serving as a useful benchmark. You don’t want to guess forever, but you also don’t have to suffer while you sort it out. Start with changes that reduce trapped body heat and remove obvious amplifiers. That gives you relief now and cleaner information for your doctor later.
Before considering any change in treatment, check with your doctor and review your complete list of side effects, as valsartan’s full profile may include symptoms like dizziness or other discomfort.
Timing is the fastest clue, and valsartan, losartan, and amlodipine are often separated by when symptoms began after a start or dose change. If your night sweats began months before valsartan, then valsartan is less likely to be the main cause. If they started within days to a few weeks of starting it, increasing it, or combining it with another drug, that points in the other direction.
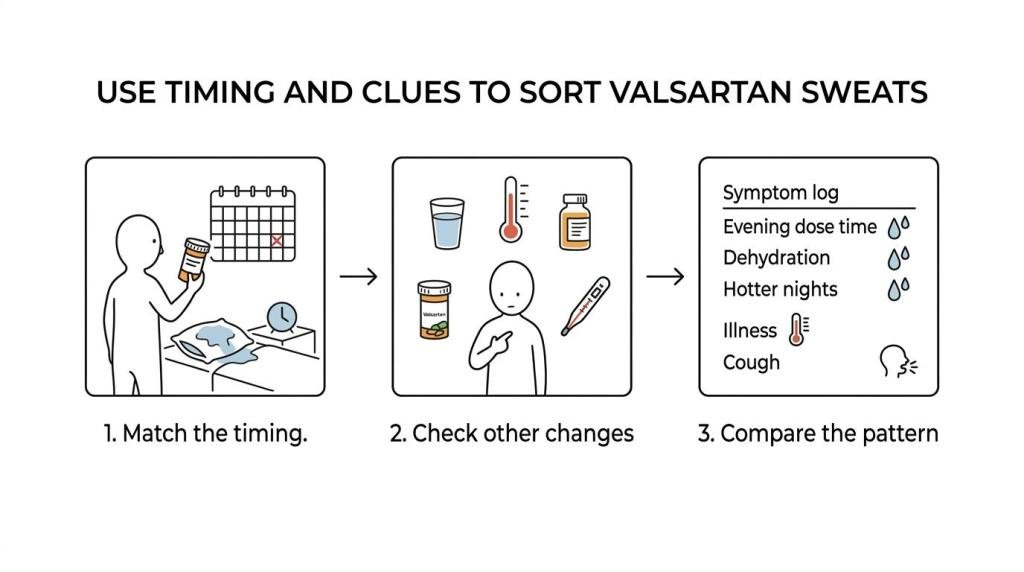
You can sort this out pretty quickly with a basic sequence:
A lot of people miss the step of checking what else changed. Valsartan may be part of the story, while another trigger might be the reason it suddenly became noticeable. Other side effects noted by patients in various studies emphasize the need to track and evaluate all symptoms.
Valsartan, losartan, and amlodipine can all be linked to sweating, although none have a reputation like venlafaxine or prednisone for causing it often. Among blood pressure medicines, the differences in side effects are usually modest. Valsartan and losartan are both ARBs, so their sweating risk profile is fairly similar in principle. Amlodipine, a calcium channel blocker, is more often associated with flushing, warmth, and ankle swelling, which some people describe as “getting hot at night.”
The bigger distinction is often the full regimen, not the single pill. If your prescription is valsartan with hydrochlorothiazide, then fluid loss can push you toward nighttime overheating more than valsartan alone.
A common misconception is that all ARBs are fully interchangeable. They are not. Dose equivalence, kidney effects, potassium levels, insurance coverage, and blood pressure response can all differ. If your valsartan controls blood pressure well and the sweating is mild, your doctor may want to improve your sleep conditions before switching medications. Remember that different patients can experience various side effects, so monitoring is important.
Yes, the pattern is often different, and menopause, anxiety, and infections like COVID-19 usually come with other clues that valsartan does not explain. Menopause-related night sweats often feel like sudden heat surges, with flushing and a strong need to throw off the covers. Anxiety can bring a racing heart, restlessness, vivid dreams, or an adrenaline jolt. Infection tends to add fever, chills, body aches, cough, sore throat, or a general sense of being unwell.
Valsartan-related sweating is more often a timing question than a syndrome, so you look for a medication change, dose timing, dehydration, and a bedroom that runs too warm. You may have sweats without fever, without body aches, and without the sense that you’re coming down with something. A good pro tip is to check your temperature when you wake up sweaty. A real temperature reading is much more useful than relying on memory alone.
A simple log of blood pressure, temperature, and symptom timing gives your clinician much better evidence than memory alone. You do not need a fancy app. Three to seven nights of notes is usually enough to make the conversation more productive. The goal is to show whether this is random, medication-linked, or pointing to another issue. Also, note if you ever have a missed dose, as that could influence the pattern of side effects.
Drenching sweats combined with chest pain, fainting, fever, swelling, or shortness of breath need prompt medical review, whether you take valsartan or lisinopril. Night sweats are often harmless, but context changes everything. If you experience low blood pressure symptoms, severe weakness, confusion, or feel like you might pass out, then the medicine may be lowering your pressure too much, or something else may be going on. For patients with hypertension, stroke risk, or kidney problems, taking extra precautions is critical.
If you have facial swelling, lip swelling, trouble breathing, or throat tightness, treat that as an urgent issue. Sweating by itself is usually not an allergy, but swelling plus breathing symptoms is a different situation. If the sweats are new and persistent, and you also have fever, cough, unexplained weight loss, swollen lymph nodes, or you just feel progressively worse, you need a medical assessment. If you have diabetes and the sweating comes with shakiness or vivid dreams, then low blood sugar should also be checked.
The simple rule is this: If sweating is the only symptom, you can usually start with tracking it and then giving your doctor a call. If the sweating comes with red-flag symptoms, act quickly. Also, if you experience further dizziness after a missed dose, contact your doctor immediately for guidance.
Before making any changes to your treatment, especially if you experience persistent side effects such as dizziness, nausea, or vomiting, speak with your doctor. Special populations, such as pediatric, geriatric patients, or those who are breastfeeding, should be monitored closely, as their responses to treatment may differ from the general population.
Targeting the bed works better than chilling the whole house, and focusing on the bed can make a big difference. Room air, tight-weave sheets, and timed airflow can cut heat buildup fast. That’s good news if energy costs are a concern. Remember, neither the bedfan nor BedJet cool the air; they only use the cool air already in the room to cool your bed.
A simple setup works best:
Remember, a colder room is not always the full answer. If your sheets trap heat, you can still wake up sweaty even when the room is at 64°F.
No, do not stop valsartan or Diovan on your own unless your clinician tells you to, because losing blood pressure control can be more dangerous than the sweating. Valsartan is often prescribed for important reasons, such as managing hypertension, heart failure, kidney protection, or post-cardiac support. Stopping suddenly can leave you with rising pressure and no real answer about what caused the sweats.
A safer plan is to call your prescriber and bring your short symptom log. Your clinician may decide to adjust the dose timing, review interactions, check kidney function and potassium, or consider a different blood pressure drug if the pattern is convincing. Remember, if you ever have a missed dose, talk to your doctor rather than trying to fix it on your own.
One more common misconception is that you need to "tough it out" until the next routine visit. You do not. If valsartan night sweats are ruining your sleep, causing dehydration, or happening with other symptoms or additional side effects, it is reasonable to contact your doctor sooner.
Taking all these precautions and tracking your side effects carefully will help ensure your safety while maintaining effective treatment for your condition.