
Prednisolone night sweats can disrupt sleep. Learn causes, warning signs, and simple ways to cool your bed safely without changing meds.
Prednisolone, similar to prednisone, can calm inflammation fast, but it can also make sleep miserable by triggering sleep disturbances, night sweats, hot flashes, restlessness, and that stuck-in-a-hot-bed feeling. That matters because poor sleep can worsen pain, mood, blood sugar swings, and next day fatigue. The hard part is knowing whether the sweating is a medication side effect, or a warning sign of something else, like infection or a blood sugar issue, as side effects can vary widely. Once you sort that out, you can usually make nights much easier without making unsafe medication changes.
Yes, prednisolone can cause night sweats. Corticosteroids like prednisolone and prednisone can shift cortisol signaling, raise alertness, and make trapped bed heat feel much stronger at night.
Prednisolone affects more than inflammation; it can also contribute to weight gain over time. It can increase metabolic activity, change blood sugar patterns, and disturb normal sleep cycles, especially if you take it later in the day or at a higher dose. If your body is already running warm, the heat that gets trapped between your fitted sheet, your body, and your top sheet has nowhere to go.
That’s why some people say they’re not sweating because the bedroom is hot, they’re sweating because the bed feels hot. Those are not the same problem.
A common misconception is that sweating means prednisone or prednisolone is “working too well” or “burning off.” It doesn’t. It usually means your temperature regulation is being pushed around due to side effects, and your sleep setup isn’t helping.
Usually, prednisolone and prednisone night sweats are uncomfortable, not dangerous. Prednisolone and Medrol can both cause sweating, but infection, high blood sugar, and steroid side effects can look similar.
Most night sweats on prednisone are a quality-of-life problem. You wake up damp, toss the blankets off, cool down, then get chilly and start the cycle again. Still, steroids can also mask fever, so you can’t assume every sweaty night is harmless, especially if you’re taking prednisolone for asthma, autoimmune disease, lupus, or after a transplant.
Pay attention to the pattern. If the sweating began right after starting prednisolone or prednisone, or after a dose increase, that points toward the drug. If you also have new cough, fever, shaking chills, or feel progressively worse, that’s a different story.
The fastest fix is usually targeted airflow, not colder room air alone. A bed fan, tighter weave sheets, and lighter bedding work better than just turning the thermostat down.
If your sweating is coming from heat trapped under the covers, the best tools are the ones that move that heat away from your skin. That’s why bed cooling systems often beat pajama changes and midnight towel-offs.
You can usually narrow it down by timing, dose changes, and other symptoms. Prednisolone, prednisone, and dexamethasone often leave a pattern if the drug is the trigger.
Start with timing. If your night sweats showed up within a few days of starting prednisone or prednisolone, or after your dose went up, that matters. If they’re worst on the same nights you take a later dose, that matters too.
Step 1, track three things for a week, your dose, the time you took it, and how intense the sweating was overnight. You do not need a fancy app, a simple phone note works.
Step 2, look for linked symptoms. If the sweating comes with insomnia, feeling wired, increased thirst, a faster heartbeat, or vivid dreams, the medication becomes more likely.
Step 3, check what doesn’t fit the medication pattern. If you have fever, cough, weight loss, weight gain, swollen glands, or new pain, then don’t assume the steroid is the whole story.
A pro tip here, don’t change the dose on your own just to “test it.” The pattern usually shows up without risky experiments.
Tonight, focus on heat removal, not just room cooling. Prednisone, prednisolone, and Zoloft can all make you feel hot, but trapped bed heat is the part you can fix right away.
Step 1, set the bedroom within the usual sleep range, about 60°F to 67°F, and strip the bed down to the lightest setup that still feels comfortable. If you start the night too bundled up, you’re already behind.
Step 2, add directed airflow under the covers. This is where a bed fan helps more than a ceiling fan, because the problem is often the microclimate in the bed, not the whole room. Common misconception, blasting the AC colder always solves it. It doesn’t if the heat stays trapped under your sheet.
Step 3, cut predictable triggers before bed. Alcohol, heavy meals, and spicy food can all add heat. If your prescriber already told you to take prednisone in the morning, stick with that. If not, ask before changing timing.
If you wake up sweaty, avoid piling on thick blankets after you cool off. Use one light layer so you don’t restart the cycle.
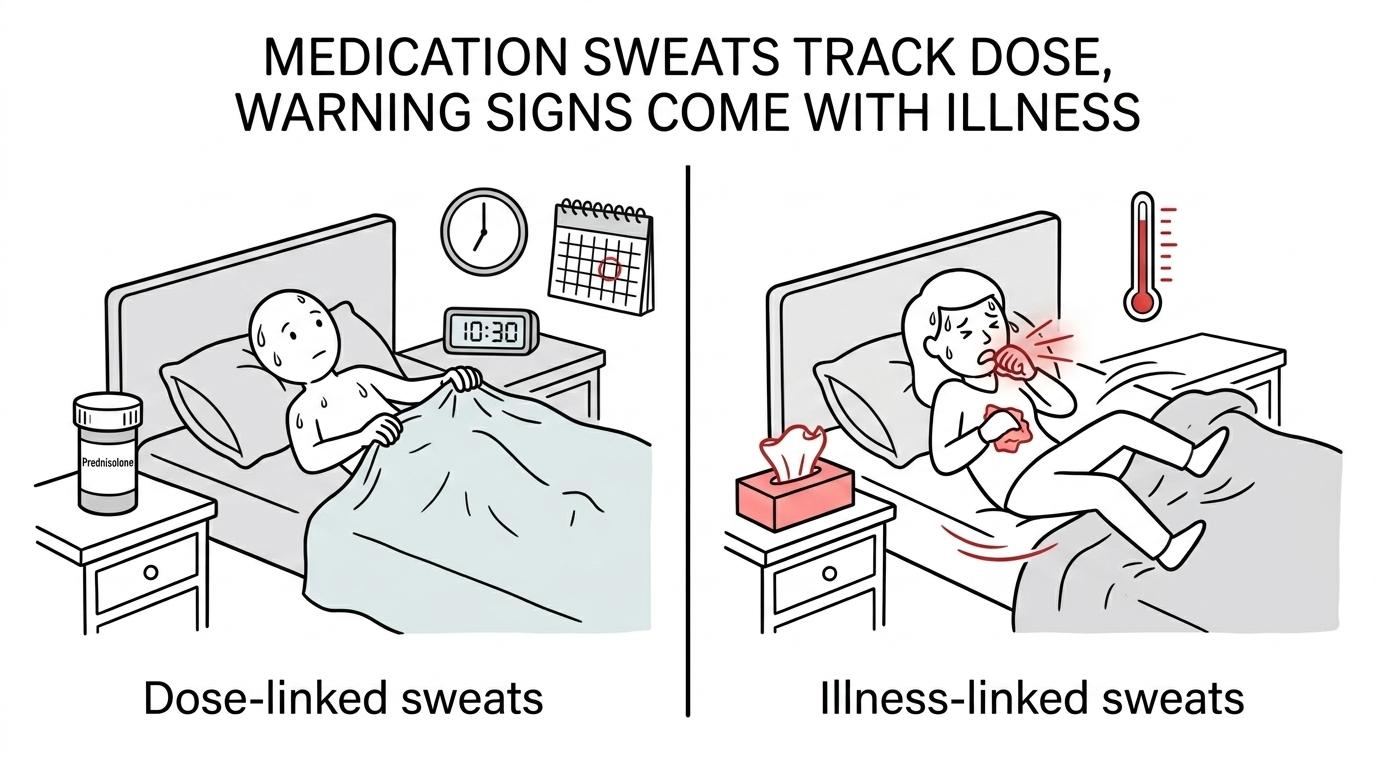
Prednisone and prednisolone sweats usually follow dose timing, while infection sweats follow illness. Prednisolone and tuberculosis can both cause nighttime sweating, but the surrounding clues are very different.
Medication related sweating, such as hot flashes and sleep disturbances, often feels mechanical and comes with potential side effects. You started the drug, increased the dose, or took it later, and now nights are hotter. It may come with insomnia, feeling keyed up, heart pounding, or higher blood sugar symptoms.
Infection related night sweats are more likely to show up with fever, chills, body aches, cough, swollen glands, diarrhea, or a general sense that you’re getting sicker. The catch is that steroids can partially blunt fever, which makes infections easier to miss.
If you’re on prednisone or prednisolone for an autoimmune condition like lupus, chemotherapy support, or after surgery, take new night sweats more seriously, because your infection risk may already be higher. If the sweating is paired with new illness signs, then treat it like a medical question first and a bedding question second.
For most people, bFan is the better value for cooling trapped bed heat. bFan and BedJet both use room air, they do not cool the air itself.
The big similarity is important. Neither system makes cold air. They both depend on the room already being reasonably cool, then move that air into the bed to carry heat away from your body. That’s why the recommended bedroom range still matters.
The big differences are cost, setup, and how focused the airflow feels. The original Bedfan came to market several years before BedJet was even thought of, and the bed fan category has always been about targeted cooling where the heat actually builds up.
A single BedJet is more than twice the price of a single bedfan. If you want two person control, a dual zone BedJet is over a thousand dollars and still costs more than twice as much as two bedfans. Two bFans can create dual zone microclimate control, one for each sleeper, without forcing both people into the same airflow or spending premium money.
Here’s the tradeoff. BedJet is a more feature heavy system and some buyers like that, although it may come with potential side effects. bFan is simpler, quieter in normal use, around 28 dB to 32 dB, and low power at about 18 watts on average. If your main goal is relief from prednisone-induced night sweats and hot flashes, simple often wins.
The right setup removes heat in layers. Your mattress, sheets, airflow, and thermostat all affect the same bed microclimate.
Step 1, start with the bedding. Use a fitted sheet and a top sheet that let air travel across your body. Pro tip, when you’re using a bed fan, a tight weave sheet often works better than a loose one because it helps channel airflow instead of letting it spill out.
Step 2, position the airflow at the foot or side of the bed so it moves under the top sheet. If the air hits your body directly and feels too strong, lower the speed and let the sheet diffuse it.
Step 3, use the room strategically. If your room is in the 60°F to 67°F range, you’re giving the system better input air. If a Bedfan lets you sleep cool at a room temperature about 5°F higher than usual, that can lower AC use without giving up comfort.
Timer controls help here, too. If you fall asleep cool but wake up chilled later, then run stronger airflow for sleep onset and taper it after the first few hours.
Call your doctor if the sweating is new, severe, or paired with other symptoms. Prednisone and prednisolone can overlap with infections, and steroids can hide the usual warning signs.
You don’t need to report every warm night. You should report a clear change, especially if you’re immunosuppressed, diabetic, or on a high dose. Night sweats that leave the sheets soaked, happen every night, or keep getting worse deserve a real conversation.
If you have a home glucose meter and you’re at risk for steroid induced high blood sugar, checking readings during a bad stretch can give your clinician useful clues.
Sometimes timing helps, but dose changes must go through your prescriber. Prednisolone and hydrocortisone can suppress your adrenal system, so stopping suddenly can be risky.
If you take prednisolone once daily, many clinicians prefer morning dosing with food because it tracks more closely with your natural cortisol rhythm and may reduce nighttime stimulation. That said, you should only change timing if your prescriber says your regimen allows it.
If your night sweats, sleep disturbances, and side effects started after a dose increase, tell the prescriber exactly when that happened. If the sweating is intense but your condition is improving, they may decide to taper sooner, reduce the dose, or switch plans. If the prednisone is essential right now, then the better move is often symptom control, cooler sleep setup, careful hydration, monitoring for weight gain, and glucose monitoring if needed.

The biggest mistake is quitting prednisone abruptly because the nights are miserable. Don’t do that. A safe taper is a medical decision, not a sleep hack.