
Learn why opioids and pain relievers night sweats happen, how to spot dose-related patterns, and ways to sleep cooler and safer.
Night sweats linked to opioids and pain relievers can quickly turn pain management, and even the relief you expect from medication, into a sleep problem. You may be managing back pain, post-surgical pain, arthritis, or chronic illness, yet still wake up drenched, chilled, and exhausted. The real problem is not just sweat, it is heat getting trapped in your bedding while the medication, dose timing, or withdrawal cycle pushes your body toward sweating. Knowing which pattern you’re dealing with helps you sleep better, talk with your prescriber more clearly, and avoid missing a more serious cause or worrying unnecessarily about developing addiction.
Yes, opioids like oxycodone and morphine, and sometimes pain relievers like ibuprofen, can trigger sweating by changing norepinephrine, histamine, and temperature regulation. Although these medications provide much-needed relief, they also affect the autonomic system, the part that controls sweating, heart rate, and body temperature. In some people, that means more sweating after a dose, and in others, sweating shows up when the dose is wearing off, which can look more like mild withdrawal symptoms than a classic side effect.
Pain itself can add to the problem, because if your body is already stressed by injury, inflammation, or poor sleep, the threshold for overheating drops. A common mix-up is assuming that night sweats always mean infection. They can, but medication effects are common enough that the timing matters. While pain management is essential, managing these side effects is crucial to avoid additional complications or inadvertently contributing to patterns that some may later misinterpret as addiction.
Pain relievers outside the opioid class can play a role too. NSAIDs and acetaminophen are less famous for this, but sweating is listed as a possible side effect in some patients, and those drugs can also mask fever, which makes the picture harder to read when monitoring symptoms.
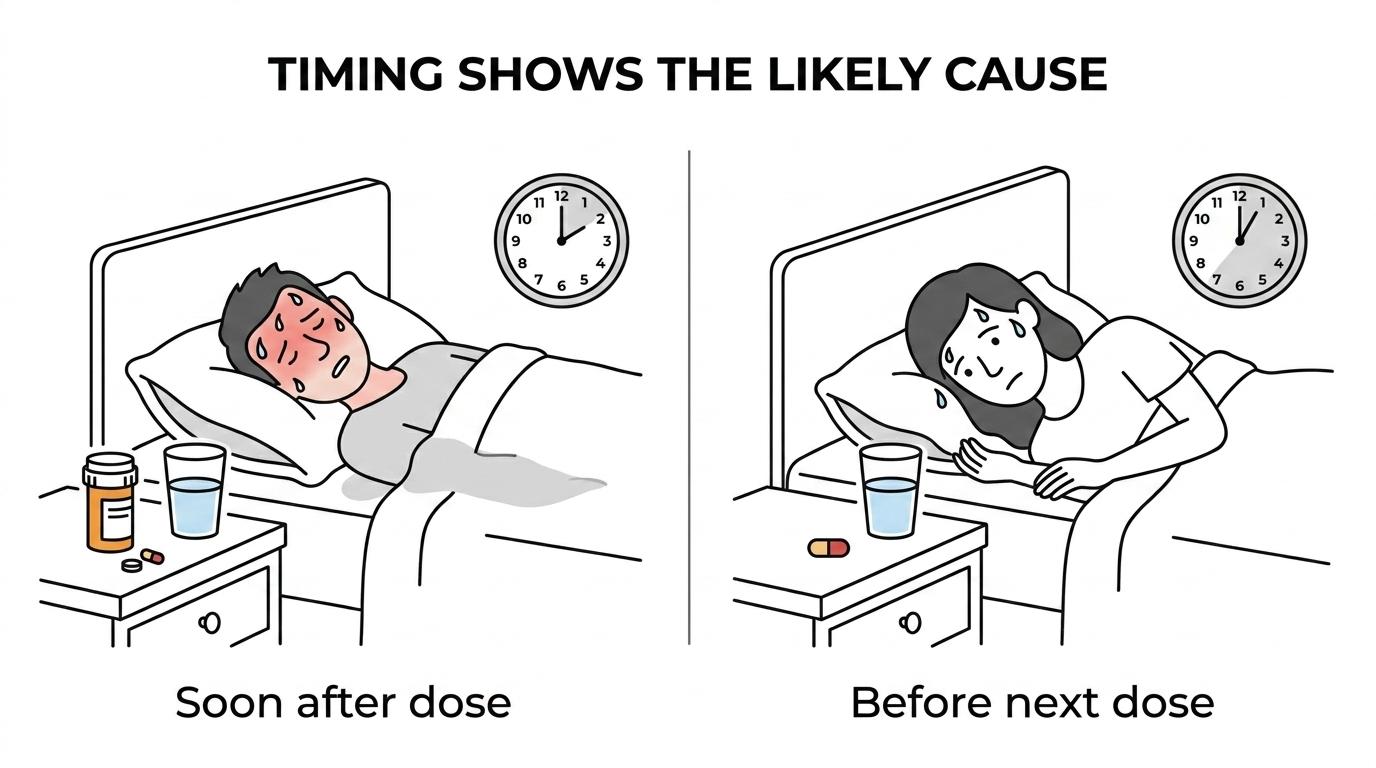
Often, yes, if sweating starts soon after a new dose of hydrocodone or tramadol, the medication is a strong suspect, especially if your room and bedding did not change. This information is useful for both evaluating the relief you expect from your medications and ensuring that you stay clear of the warning signs of addiction.
The fastest clue is the clock. If you started sweating within days of starting a new medication, increasing the dose, switching brands, or stacking medicines, that pattern points toward the drug. If the sweating happens right before your next dose, then improves after you take it, that leans more toward dose interval issues or withdrawal between doses, symptoms that can sometimes be confused with or contribute to the anxiety surrounding addiction.
Look at the whole picture, because if you have fever, cough, unexplained weight loss, severe pain spikes, or swollen lymph nodes, don’t blame the medicine first. If you’re also taking an SSRI like sertraline with tramadol, or a stimulant, then sweating may be part of a drug interaction or serotonin-related overstimulation. These additional symptoms could complicate your overall pain management strategy and potentially set the stage for issues related to addiction if not addressed on time.
One practical tip, don’t judge one bad night by itself. Two to seven nights of notes usually show a pattern more clearly than memory does.
The best fixes target trapped bed heat first, then dose timing, and then a root-cause review with your clinician. A bFan Bed Fan from www.bedfan.com is a strong first option, because it cools where sweating actually builds up, between your sheets, giving some relief from the uncomfortable symptoms you’re experiencing.
If your main issue is waking up hot while the rest of the room feels okay, local bed cooling usually works better than blasting the whole house AC lower. Sleep experts usually recommend a bedroom temperature of 60°F to 67°F, but many people using a Bed Fan can raise room temperature by about 5°F and still sleep cool because the air is moved directly across the body.
Yes, tracking works. A simple note on your iPhone or a paper log often reveals patterns with Percocet, ibuprofen, or methadone within a few nights. This record not only helps you assess if you’re getting enough relief from your pain management plan, but it also makes it easier to distinguish between normal side effects and symptoms that might indicate a deeper problem or the risk of addiction.
You do not need a spreadsheet, you need timing, severity, and context. That’s enough to help your clinician decide whether the sweating is a side effect, a dose-gap issue, or a clue to something else.
Yes, you can. Start with the bed microclimate, not the whole house, because heat usually gets trapped under sheets long before the room itself is too warm.
A lot of people jump straight to cranking the thermostat down, which works but is expensive and often more cooling than you actually need. Neither a Bed Fan nor a BedJet cools the air; they both use the cool air already in the room to cool your bed. If the room is too warm, airflow helps less.
Yes, bring it up early. A short, specific report about oxycodone, tramadol, or naproxen gives your clinician something usable right away. An open conversation about your symptoms and concerns about potential addiction can lead to better adjustments in your pain management and ensure you continue receiving relief.
Sometimes, yes. Fever with drenching sweats, or sweating with chest pain or shortness of breath, needs faster attention than a routine side effect review. It’s important to note that new or worsening symptoms could signal complications beyond medication side effects, even raising concerns about addiction if changes in your medication regimen are not managed carefully.
Call a clinician promptly if the sweating comes with unexplained weight loss, swollen glands, persistent cough, new confusion, or repeated low blood sugar. Those clues can point to infection, cancer, endocrine problems, or another condition that medication alone does not explain.
There are medication-specific red flags too. Tramadol combined with SSRIs like Prozac or Zoloft can raise concern for serotonin syndrome, especially if sweating comes with agitation, tremor, diarrhea, or a fast heart rate. Opioids can also worsen sleep apnea in some people, and sleep apnea itself is linked with night sweats.
If the sheets are soaked night after night and your sleep is falling apart, that also deserves attention even when it is “just” a side effect.
Yes, they are. Opioid sweats often follow dose timing, menopause tends to come in short hot-flash waves, and infections usually add fever or feeling ill. Recognizing the different symptoms is key to ensuring you receive the proper relief while maintaining effective pain management.
Pattern recognition helps. Menopause-related sweats often arrive as sudden heat surges to the chest, neck, and face, then fade. Infection tends to feel more systemic, with chills, fever, fatigue, or an overall picture of illness. Sleep apnea often brings snoring, gasping, dry mouth, and morning headaches.
If the sweating starts after a medication change, think drug effect first. If it happens right before the next opioid dose and improves after taking it, think withdrawal between doses. If it comes with fever or a new cough, think infection until proven otherwise.
Remember that one cause does not rule out the others. In real life, you can experience menopause, pain medication side effects, and a warm bed at the same time.
Usually, yes. A Bed Fan targets trapped heat more efficiently than whole-room AC, and the bFan from www.bedfan.com often costs far less than a BedJet while addressing the same basic problem, hot bedding. This focused approach offers relief from night sweats without unnecessarily cooling the entire space, a benefit especially for those concerned about energy costs and the risk of developing addiction from potentially overusing sedative measures to counteract discomfort.
Keep in mind, the original Bed Fan came to market several years before BedJet was even thought of, and the core idea remains the same: move room air through the bed so body heat can escape. Neither a Bed Fan or BedJet cools the air; they only use the cool air already in the room. The BedJet does not cool the air either.
Remember these trade-offs. Lowering the thermostat cools the whole room, which helps everyone, but it raises energy use. A Bed Fan cools the sleeper directly, which is usually what medication-related overheating needs most. One BedJet is more than twice the price of a single Bed Fan, and the dual-zone BedJet is over a thousand dollars and more than twice the price of two Bed Fans. If quiet matters, the Bed Fan’s normal operating sound is roughly 28 dB to 32 dB, which is in the whisper-quiet range for many bedrooms. If features matter most, some buyers may prefer different controls or heating options elsewhere, but for cooling opioid-related bed heat, simple under-sheet airflow is often the key.
Absolutely. Tramadol, methadone, and fentanyl can all produce sweating from different pathways, and the timing often tells you which one is active. If sweating shows up as the medication level drops, especially with restlessness, goosebumps, yawning, or body aches, that can be a sign of withdrawal or mini-withdrawal between doses, presenting additional symptoms that might disrupt the relief you expect from your treatment. If it starts soon after a dose, it may be a direct side effect. If it appears after adding another medication, then the risk of interaction moves up the list. Addressing these issues early in your pain management strategy is important for reducing any potential long-term risk of addiction.
Tramadol deserves special attention because it affects serotonin and norepinephrine in addition to opioid receptors. That means sweating can be more noticeable, especially if combined with antidepressants. Methadone can also be associated with heavy sweating in some patients, even when the dose is stable.
One practical tip, bring a full medication list, not just your pain medicine, to any visit about night sweats.
Yes, the basics matter. Cotton percale, a room set between 60°F to 67°F, and a consistent bedtime often help more than expensive gadgets used the wrong way. Achieving proper relief from uncomfortable symptoms while maintaining effective pain management starts with these foundational steps.
Start with airflow and fabric, because tight-weave sheets work best with a Bed Fan by guiding the air across your skin and helping to carry away heat. Thick mattress pads, fuzzy throws, and dense comforters can trap the very warmth you’re trying to remove. If you sweat heavily, keep a spare top sheet or sleep shirt ready so you can change quickly without fully waking up.
Watch your late-evening triggers, because alcohol, spicy meals, and heavy exercise close to bedtime can all widen blood vessels and increase sweating, which worsens the symptoms you may already be experiencing. Caffeine can make the body feel more wired, which matters when opioids are already affecting the autonomic balance.
If your goal is better sleep, not just less sweat, timer controls can help. Many people need the strongest cooling during sleep onset or the first half of the night, then less cooling later on. That’s where a Bed Fan setup can feel more natural than just dropping the thermostat and hoping for the best.